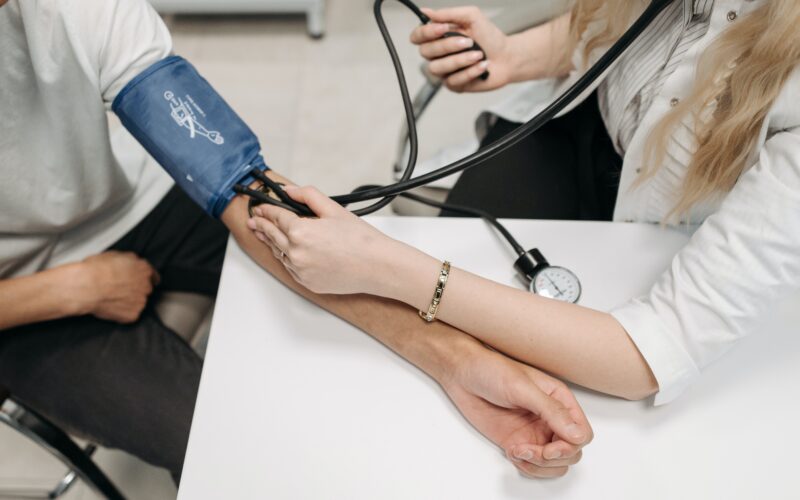
The launch of a rural health strategy is a chance to finally address many of the health discrepancies facing rural communities, the Rural Health Network says.
Jeremy Webber, the clinical director of the Rural Health Network (Hauora Taiwhenua), said he is hopeful it will address issues such as a shortage of health professionals working in rural practices and improve access to services.
“This gives us hope, which is something we haven’t had in a long time in rural health.”
He welcomes the fact that the strategy is ambitious, saying it needs to be bold to fundamentally address current issues rather than be another Band-Aid solution.
The strategy, initiated by the Ministry of Health, sets the direction for improving the health and wellbeing of rural communities over the next 10 years.
“Our vision is for all people living in rural communities to live long and healthy lives, supported by a health system that meets the varied needs of these communities and draws on the strengths and knowledge of rural communities to achieve pae ora – healthy futures,” a spokesperson said.
The strategy prioritises rural communities with the aim of providing services that meet their needs rather than adapting those designed for urban settings.
Another focus is to provide more preventative health interventions, such as screening, and to promote health and wellbeing.
It also aims to provide services closer to those living in rural communities through health providers, outreach programmes and digital options, but if this is not possible, communities must be supported to travel to access services.
The final priority is to grow and support the rural health workforce.
“Making sure rural roles are better valued and supported is a key part for attracting and retaining our people,” the spokesperson said.
That includes creating career pathways and increasing interdisciplinary rural placements to attract more people into rural health.
The spokesperson said the needs of rural communities are often under-served by access to services, especially for remote communities and rural Māori, and a focus is to remove geographic differences in care and outcomes.
“The different needs of rural communities have not been considered in funding and planning health services, and rural health outcomes were not monitored like other population groups,” the spokesperson said.
Webber said the network was consulted in the development of the strategy.
His hope is that in five years there will be a marked improvement in the number of clinicians wanting to work in rural practices, seeing it as a rewarding and stimulating career, enhanced by improved training systems.
One of the issues the strategy aims to address is improving vaccination rates for rural two-year-olds, which are lower than in urban areas.
A University of Otago study released last week found amenable mortality rates for rural people were in some demographics twice that of those in urban areas.
The study found results were worse for those aged under 30 living in the most rural communities, where mortality rates were double that of the most urban centres at 599 urban deaths per 100,000, compared with 1085 rural.
The spokesperson said the study confirms findings in Australia, Canada and the United States, where rural mortality exceeds urban.
“We know that reasons for this disparity is complex and affected by several factors, such as socioeconomic status and ethnicity, but also access to health care and experiences people have when receiving care.”