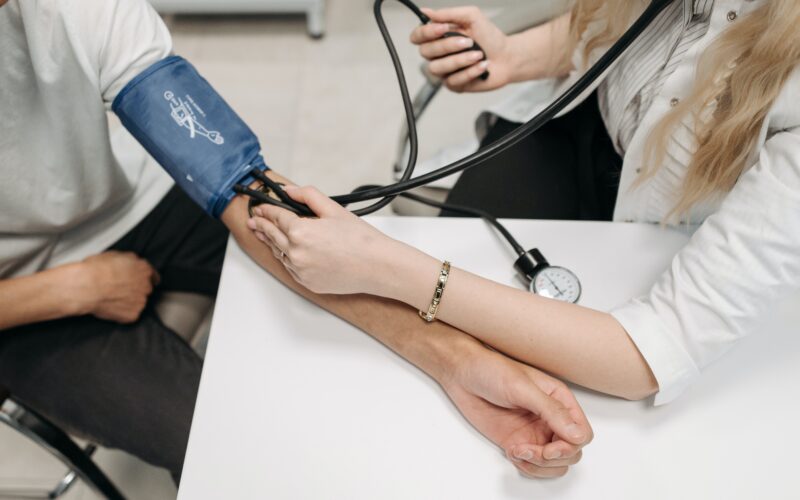
State of Rural Healthcare

About this special report
In an ongoing series, Neal Wallace takes a look at the dire state of rural healthcare in New Zealand, the challenges rural communities face from a shortage of medical professionals and access to services but also the measures being taken to rectify the situation.
Pay deal could worsen rural nursing shortage
New equity agreements exclude those working in community and primary facilities.
South Otago rural health entities join forces
Five services sign up to ‘collaborative network’.
Rural Health Network welcomes new strategy
‘Vision is for all people living in rural communities to live long and healthy lives’.
Study flags higher mortality in rural NZ
Under-30s in the most rural communities are dying twice as fast as city peers.
Network welcomes ‘mighty first step’ for rural health
Workforce plan and election promise ‘reflect our thinking'.
Bringing health services to rural women
A Dunedin gynaecologist sold her home to fund a bus that brings better health care to women in remote areas.
Review urged to look at helivac funding
Feds hopes health audit will also address inequity in rural-urban health provision.
Health NZ reviews rural after-hours care
Increasing numbers of patients choppered to towns.
Helicopter health filling rural gap
First responders increasingly relied on to meet need.
Minister praises rural health ‘resilience’
Sector has challenges but is not collapsing, says Prime.
Reti flags ‘resigned desperation’ of rural GPs
National’s health spokesperson says former colleagues are exhausted.
100 rural GP posts empty for a year
In the interim, communities have found their own solutions such as a mobile healthcare facility to assist women.
Rural GP practice delivers joys and trials
It’s not all tough going, recalls long-serving rural doctor.
Admin absurdity is driving Clutha’s health staff away
Community-owned healthcare provider Clutha Health First is typical of the frustrations faced by rural health providers.
Rural health frontline workers feel ‘misunderstood, frustrated’
Small rural hospitals, often the only source of healthcare for the 25% of New Zealanders who live in rural areas, are feeling neglected, misunderstood, frustrated and burnt out.
Doctors taking strain as rural health shortages persist
Survey finds rural hospital doctors feel even more overworked than a year ago.
More Special Reports
 Cyclone Gabrielle: After the Flood
Cyclone Gabrielle: After the Flood Cyclone Gabrielle: Rebuilding Land and Lives
Cyclone Gabrielle: Rebuilding Land and Lives Cyclone Gabrielle: Road to Recovery
Cyclone Gabrielle: Road to Recovery Dairy Input Costs
Dairy Input Costs Dairy South
Dairy South Dairy's Decade Ahead
Dairy's Decade Ahead DIY Soil Health
DIY Soil Health Farms, Forests and the Future
Farms, Forests and the Future Food Security
Food Security Future of Sheep Farming
Future of Sheep Farming Jaded Leadership: Time to Regroup
Jaded Leadership: Time to Regroup Rural Leadership
Rural Leadership Spotlight on Drench Resistance
Spotlight on Drench Resistance Spotlight on Labour
Spotlight on Labour State of Rural Healthcare
State of Rural Healthcare Succession: How to step back successfully
Succession: How to step back successfully Unpacking NZ's Ag Policy Drive
Unpacking NZ's Ag Policy Drive